Dental disease is the single most underdiagnosed condition in companion animals. Studies consistently show that over 80% of dogs and 70% of cats over the age of three have some degree of periodontal disease — yet most of these animals are never brought to the vet specifically for their teeth. In India, this figure is likely higher: homemade diets heavy in soft, sticky, carbohydrate-rich food, year-round humidity that accelerates bacterial growth, and the widespread belief that dental care is optional combine to create a population of pets with severe, painful, and entirely preventable oral disease.
The consequences extend far beyond bad breath. Advanced periodontal disease is a chronic bacterial infection in the mouth. The same bacteria that destroy gum tissue and bone enter the bloodstream through damaged oral mucosa, seeding the kidneys, liver, and cardiac valves. The link between severe periodontal disease and subclinical kidney disease and cardiomyopathy in dogs is well-established. Dental care is not cosmetic — it is systemic health maintenance.
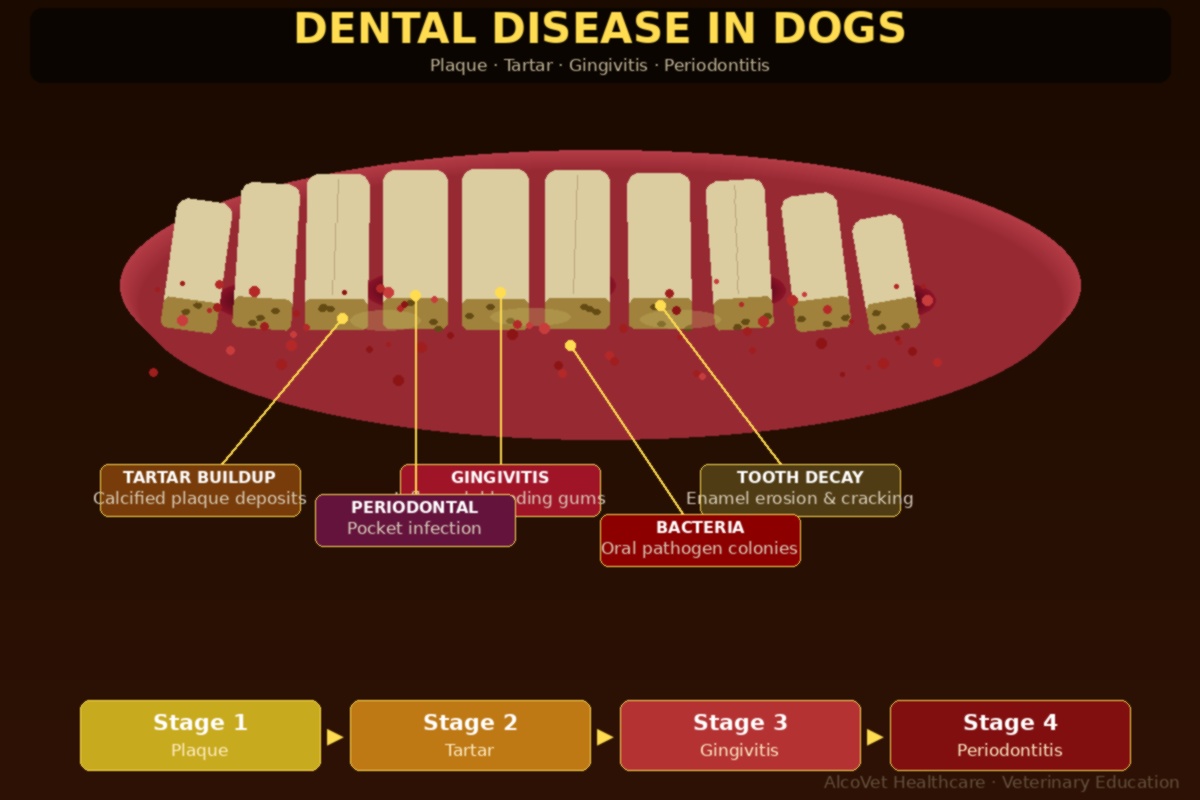
The Four Stages of Periodontal Disease
Periodontal disease is progressive and largely irreversible. Once bone loss around the tooth root occurs (Stage 3+), it cannot be regenerated. Understanding the staging helps you act before the damage becomes permanent.
Clean Teeth, Healthy Gums
No plaque or tartar. Gums are pale pink, firm, and do not bleed on touch. This is where preventive home care keeps your pet — the goal of daily brushing.
Plaque + Early Gum Inflammation
Plaque accumulates along the gumline. Gums become red and slightly swollen. Fully reversible with proper cleaning and improved home care. No bone loss yet.
Tartar, Pocket Formation, <25% Bone Loss
Hardened tartar on tooth surfaces. Gum pockets begin forming around tooth roots. Early bone loss begins. Partially reversible with professional cleaning. Home care becomes critical to slow progression.
Deep Infection, Tooth Mobility, Abscess
25–50%+ bone loss. Deep gum pockets with active infection. Teeth become mobile and painful. Root abscesses form — bacteria enter bloodstream here. Irreversible bone loss; extraction often the only humane option. Systemic organ effects begin at this stage.
Signs of Dental Disease — What to Look For
Pets instinctively mask pain, including dental pain. By the time a dog or cat refuses food or cries when eating, the disease is typically severe. The earlier signs are subtle and easily missed without a deliberate monthly oral check.

Feline Tooth Resorption — A Cat-Specific Emergency
Tooth resorption (formerly called feline odontoclastic resorptive lesions, or FORLs) is one of the most painful dental conditions in cats and is severely underdiagnosed in India. It affects an estimated 28–67% of cats and is not caused by diet alone — it is a progressive, idiopathic destruction of tooth structure from within. The odontoclast cells that normally resorb baby teeth abnormally reactivate and begin destroying adult teeth.
The lesions typically begin at the gumline, creating a notch or cavity at the tooth neck that is extremely sensitive. They are invisible without dental radiography — a cat can have severe, intensely painful resorptive lesions without any visible tartar or gum disease. Cats almost never vocalise from dental pain; the only signs are typically subtle: reduced grooming around the face, jaw chattering when yawning, slight weight loss, or mild food preference change.
Daily Home Dental Care — The Brushing Protocol
Tooth brushing is the most evidence-supported home dental care intervention. It physically disrupts the plaque biofilm that forms on tooth surfaces within 24 hours of cleaning. Studies show that brushing at least every 48 hours significantly reduces plaque scores; daily brushing is ideal. The technique matters as much as the frequency.
Step-by-Step Brushing Guide
- 1Choose the right toothpaste. Use only enzymatic pet toothpaste — the enzymes (glucose oxidase, lactoperoxidase) disrupt plaque bacteria chemistry even without perfect mechanical brushing. Never use human toothpaste — fluoride is toxic to pets if swallowed, and the foaming agents (SLS) cause gastric upset. Chicken, beef, and malt flavours are available and improve acceptance significantly.
- 2Start with taste alone for the first week. Let your pet lick the toothpaste off your finger before attempting any brushing. The goal is creating a positive association with the taste and the dental routine before adding any mechanical manipulation.
- 3Begin with a finger brush. A silicone finger brush gives you better tactile control and is less confrontational than a handled toothbrush. Apply a pea-sized amount of toothpaste and gently rub along the outer surfaces of the upper back teeth — this is where tartar accumulates fastest.
- 4Focus on the gumline at a 45-degree angle. The bristles should angle slightly toward the gumline — where plaque-to-tartar conversion begins. Use small, gentle circular motions rather than long strokes. You do not need to brush inner tooth surfaces — the tongue provides some mechanical cleaning there.
- 5Transition to a soft-bristle toothbrush at 2–3 weeks. A pet-specific soft toothbrush reaches into gum pockets better than a finger brush for dogs; for cats, small-headed brushes or even a gauze pad around your finger work well.
- 6Always end with a high-value reward. A small treat, praise, or play immediately after brushing reinforces the behaviour powerfully. Dogs and cats can learn to actively look forward to brushing if the ending is consistently positive.
- 7Aim for daily brushing; 3–4 times/week is acceptable. Below twice weekly, the plaque-disruption benefit drops significantly. If your pet actively resists despite desensitisation, discuss alternatives with your vet — some adjunct products offer partial benefit for resistant animals.

Dental Products — Evidence and Effectiveness Guide
A wide range of dental products are available in India for pets. Effectiveness varies significantly — VOHC (Veterinary Oral Health Council) approval is the most reliable indicator that a product has been independently tested for plaque or tartar reduction claims.
| Product Type | How It Works | Evidence Level | Key Notes for India |
|---|---|---|---|
| Enzymatic toothpaste + brushing | Mechanical plaque disruption + enzymatic bacterial inhibition | Highest — gold standard | Chicken/beef flavour options available; do not substitute human toothpaste |
| VOHC-approved dental chews (Greenies, OraVet, Pedigree Dentastix) | Mechanical abrasion as chewing action shears plaque from tooth surfaces | Good — adjunct, not replacement for brushing | Must be appropriately sized; risk of oesophageal obstruction if swallowed whole; not appropriate for aggressive chewers |
| Water additives (TropiClean, Healthymouth) | Antimicrobial agents (cetylpyridinium chloride, zinc) reduce bacterial load in saliva | Moderate — better than nothing; less effective than brushing | Good option for cats and brush-resistant pets; add to fresh water daily; some pets refuse flavoured water |
| Dental diets (Hill's t/d, Royal Canin Dental) | Kibble shape and texture designed to provide abrasive cleaning as the tooth sinks in before breaking | Good — VOHC-approved options exist | Requires exclusive feeding to be effective; less accessible in India; not suitable for all life stages |
| Oral gels (Oratene, Vetri-Science) | Enzymatic and antimicrobial agents applied directly to gum surfaces | Moderate — useful for cats and small dogs | Can be applied with a finger or Q-tip; good for post-surgical oral care |
| Seaweed supplement (PlaqueOff) | Ascophyllum nodosum algae — mechanism not fully elucidated; reduces plaque tackiness | Emerging — some clinical evidence | Added to food daily; available online in India; safe and palatable for most pets |
| Raw bones | Mechanical abrasion — some evidence for plaque reduction | Controversial — risks outweigh benefits for most pets | Fracture slab teeth (carnassial fracture is very common), cause GI obstruction, carry Salmonella; not recommended by most veterinary dental specialists |
Professional Veterinary Dental Cleaning
Home care slows progression but cannot remove established subgingival tartar — the mineralised plaque that has migrated below the gumline into the periodontal pocket, where active bone destruction occurs. This requires professional scaling under general anaesthesia. Anaesthesia-free dental cleaning, which is offered by some groomers and non-veterinary providers in India, is ineffective and potentially harmful — it only cleans visible tooth surfaces without addressing the subgingival disease, while stressing the animal and providing false reassurance to the owner.
What Happens During Professional Dental Cleaning
- Pre-anaesthetic bloodwork: Liver and kidney function assessment — essential before any GA, and particularly important in pets over 6 years
- Full-mouth dental radiography: X-rays of every tooth including the roots — this is the only way to identify resorptive lesions, root fractures, and bone loss below the gumline; any dental cleaning without radiography is incomplete
- Ultrasonic scaling: Removes supragingival (above gumline) and subgingival (below gumline) tartar from all tooth surfaces
- Subgingival curettage: Manual removal of tartar from within periodontal pockets using hand instruments
- Polishing: Smooths tooth enamel surface to slow plaque re-adhesion
- Extractions: Non-viable teeth — those with severe bone loss, resorptive lesions, or root fractures — are extracted under anaesthesia with local nerve blocks for pain management
- Post-procedure care: Prescription antibiotics or pain relief if extractions were performed; soft food for 5–7 days post-extraction
Common Dental Myths in India — Corrected
India-Specific Dental Health Considerations
When to See the Vet Urgently
Related Guides
This content is provided for educational purposes only and is not a substitute for professional veterinary advice, diagnosis, or treatment. Dental disease assessment requires hands-on oral examination and, for cats especially, dental radiography under general anaesthesia. If your pet shows any signs of oral pain or dental disease, contact your registered veterinarian for a dental examination. Do not attempt to extract or treat teeth at home.
