Third Eyelid (Cherry Eye) Surgery Care for Dogs

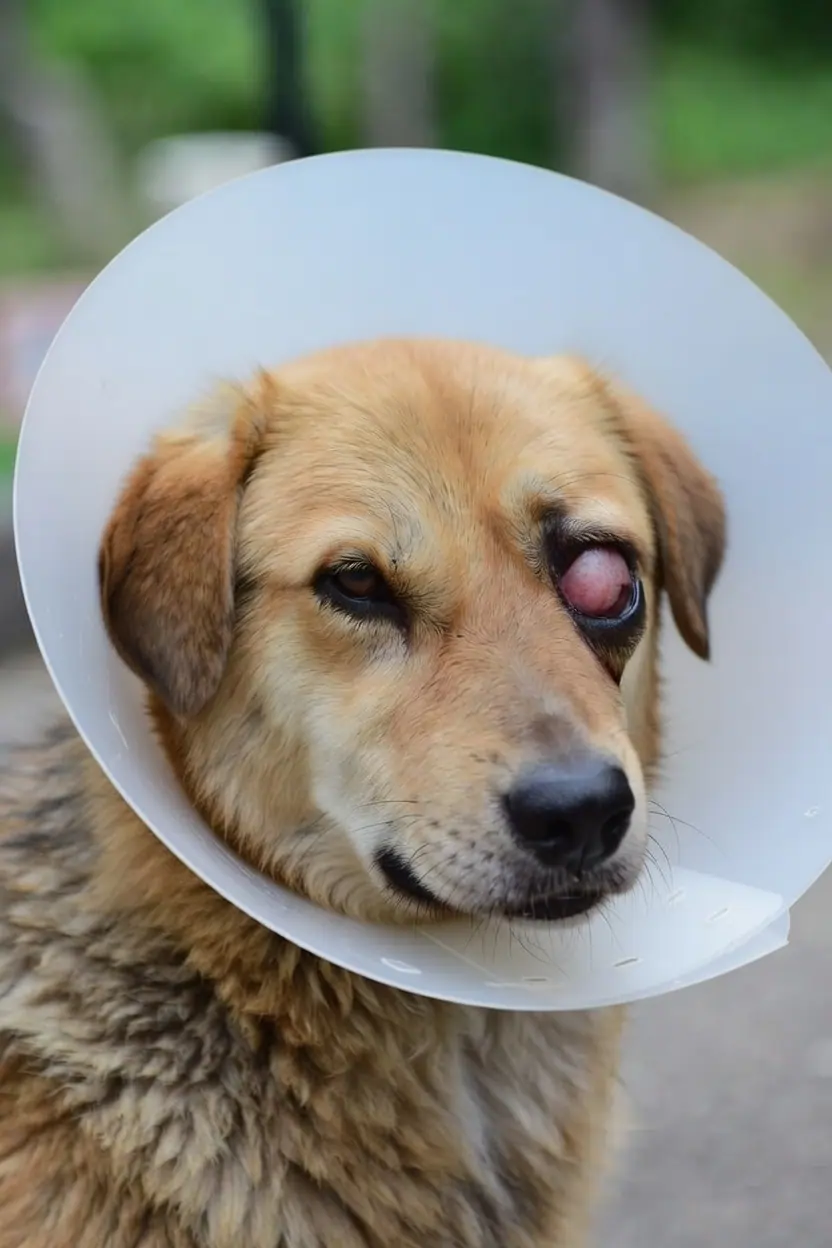
What is cherry eye?
Cherry eye is the prolapse of the nictitans gland — the secretory gland housed within the third eyelid (nictitating membrane). It appears as a smooth, round, red or pink mass protruding from the inner corner of the eye and is most common in young dogs under two years of age.
The condition is rarely painful in the early stages but can lead to conjunctival irritation, discharge, exposure dryness and, if untreated or mismanaged, a significantly increased lifetime risk of keratoconjunctivitis sicca (KCS / dry eye).
Breeds most commonly affected
Cherry eye has a strong breed predisposition linked to weak connective tissue anchorage of the nictitans gland. Breeds at highest risk include:
Cherry eye is bilateral in up to 40–50% of cases in predisposed breeds. If one eye is affected, the fellow eye should be monitored carefully and owners counselled about the risk of bilateral involvement.
Surgical technique comparison
Modern cherry eye surgery aims to reposition the gland rather than remove it. The nictitans gland contributes 30–50% of total basal aqueous tear production — excision is strongly associated with lifetime KCS risk.
| Technique | Principle | KCS Risk | Recurrence | Current Status |
|---|---|---|---|---|
| Morgan Pocket Technique | Gland buried in a conjunctival pocket and sutured | Low | 5–15% | Preferred |
| Imbrication / Anchoring | Gland anchored to periorbital tissue via suture | Low | 10–20% | Preferred |
| Combined Pocket + Anchor | Dual fixation — used in brachycephalic breeds | Low | 5–10% | Preferred |
| Gland Excision | Complete surgical removal of nictitans gland | Very High | N/A — gland absent | Avoid |
| Manual Replacement | Non-surgical digital reduction | Low | Very high | Temporary only |
If excision was performed: Lifelong aggressive lubrication and regular STT monitoring are essential. Discuss cyclosporine or tacrolimus prophylaxis with your veterinary ophthalmologist to delay or prevent KCS onset.
Post-operative recovery — phase by phase
The following is a general educational guide. Always follow your veterinary surgeon's specific post-operative instructions.
Immediate post-operative period
- E-collar worn continuously — essential to prevent suture disruption
- Expect mild periocular swelling, redness and serous discharge — normal
- Anti-inflammatory / antibiotic drops (FurrMoxi LP if corneal integrity confirmed) 3–4× daily
- Lubricant (Vet Tears HA) Q3–4H to maintain surface hydration
- No bathing; keep eye away from dust and foreign material
Early healing phase
- Swelling should begin to resolve by day 5–7; discharge reduces
- Continue medicated drops as prescribed; begin taper at day 10 if healing on track
- Continue lubricant 3–4× daily
- E-collar remains essential until sutures are fully healed
First post-operative recheck — STT assessment
- Schirmer Tear Test performed — critical to identify post-operative tear reduction
- Suture assessment; discharge should be minimal by now
- Taper or discontinue medicated drops based on healing status
- Adjust lubricant frequency based on STT result (see table below)
Consolidation and long-term planning
- Second STT to confirm tear production stability
- Lubricant continued at maintenance frequency based on STT
- If STT remains low (<10 mm/min), discuss cyclosporine or tacrolimus with your vet
- Predisposed breeds: schedule STT every 3–6 months ongoing
Post-operative STT monitoring guide
The Schirmer Tear Test at week 2 is the most important post-cherry eye surgery check. Use these values as a general guide — your veterinarian will tailor management to your individual patient.
| STT at Wk 2 | Interpretation | Recommended Action |
|---|---|---|
| ≥ 15 mm/min | Normal — gland functioning well | Taper lubricant to 2× daily; recheck at week 6 |
| 10–14 mm/min | Borderline — monitor closely | Continue lubricant 3–4× daily; recheck at week 4 |
| 5–9 mm/min | Low — post-operative KCS risk | Lubricant 4–5× daily; initiate cyclosporine 0.2% BID; recheck at week 4 |
| < 5 mm/min | Very Low — urgent attention needed | Lubricant Q2–3H; aggressive immunomodulator therapy; consider specialist referral |
Role of ocular lubricants in cherry eye recovery
Sodium hyaluronate-based lubricants restore tear film stability, reduce corneal surface friction and support epithelial integrity during the post-operative window when gland function may be temporarily impaired. They are safe for high-frequency use and do not interfere with wound healing.

Managing inflammation and infection risk
Post-operative inflammation is expected and best managed with a short course of anti-inflammatory cover. Where secondary infection risk is present, combined antibiotic-steroid preparations provide dual protection under veterinary supervision.
Critical safety rule: Steroid-containing ophthalmic preparations are contraindicated in active corneal ulceration. Always confirm corneal integrity with fluorescein staining before prescribing any steroid eye drop post-operatively.
Warning signs — contact your vet immediately
Seek urgent veterinary attention if you observe:
- Re-prolapse of the gland — the red mass reappears in the eye corner
- Marked worsening of swelling or pain beyond day 3–4
- Purulent (thick yellow/green) discharge
- Corneal cloudiness, bluish haze or sudden vision changes
- Pet rubbing the eye or managing to remove the e-collar
- Visible suture dehiscence or wound opening
Home care checklist
- Keep e-collar on at all times — including during sleep and feeding
- Apply drops using the lower eyelid pouch technique — do not touch cornea with dropper tip
- Apply medicated drop first, wait 5–10 min, then apply lubricant
- Gently clean discharge with sterile saline-dampened gauze — wipe outward only
- Avoid bathing, swimming or dusty environments during recovery
- Restrict jumping and rough play in the first 2 weeks
- Store eye medications correctly — some require refrigeration
- Attend all scheduled rechecks — even if the eye looks well
Frequently Asked Questions
What is cherry eye in dogs?
Cherry eye is prolapse of the nictitans gland — the tear-secreting gland within the third eyelid. It appears as a smooth red or pink mass at the inner corner of the eye and is most common in young dogs of brachycephalic or predisposed breeds. Surgical repositioning is the standard of care.
Which breeds are most prone to cherry eye?
Cocker Spaniel, English Bulldog, Beagle, Basset Hound, Lhasa Apso, Shih Tzu, Pug, Bloodhound, Shar Pei and Boston Terrier are among the highest-risk breeds. It is especially prevalent in dogs under two years and may affect both eyes in up to 40–50% of cases in predisposed individuals.
Why is the gland not just removed?
The nictitans gland contributes 30–50% of basal aqueous tear production. Removal dramatically increases the lifetime risk of KCS (dry eye disease), which requires lifelong management and significantly reduces quality of life. Modern pocket and anchoring techniques reposition the gland effectively while preserving its function.
Does cherry eye surgery affect tear production?
Surgery may temporarily reduce tear output. A Schirmer Tear Test at week 2 is essential to detect this early. If STT is low (<10 mm/min), a lubricant protocol adjustment and consideration of immunomodulatory therapy significantly reduce the risk of progression to permanent KCS.
Are lubricating eye drops used after cherry eye surgery?
Yes — routinely. Sodium hyaluronate-based lubricants such as Vet Tears HA are recommended from day one post-operatively to maintain surface hydration, reduce friction and protect the corneal epithelium while the gland recovers its secretory function.
How long does recovery take after cherry eye surgery?
The acute phase is 2–3 weeks. Lubricant use and STT monitoring continue for 4–6 weeks. In predisposed breeds, routine STT monitoring every 3–6 months is advisable long-term, as the risk of KCS remains elevated even after successful surgery.
Can cherry eye come back after surgery?
Yes — recurrence is possible, particularly in brachycephalic breeds and following the pocket technique alone. Recurrence rates of 5–20% are reported depending on technique and breed. Re-operation using a combined pocket-plus-anchor approach is often successful in recurrent cases.
Explore related eye care guidance
Disclaimer: This page is for general informational and educational purposes only. It does not replace professional veterinary diagnosis, clinical examination or post-operative care instructions from your veterinary surgeon. AlcoVet Healthcare assumes no liability for actions taken based on the content of this page.
